 These examples are based on the medical instructions for use from Västmanland Hospital Västerås, in Sweden where the project originated. While every health care provider utilising SHFNO will need to ensure that they have medical instructions for use in place, these guidelines are provided as an example, which is subject to change and without any liability ( see Legal Disclaimer). We further recommend against using SHFNO for patients with confirmed secondary bacterial infections as well as for carriers of drug-resistant bacteria. Even so, it is the authors' suggestion that the only patients eligible for treatment with Split HFNO (Hereon " SHFNO") are patients suffering from the same disease, such as COVID-19, which also means that potential cross-bcontamination across patients is less significant. The unidirectionality of the air flow means that no air is shared between patients, even without added filtration. This is due to the open nature of the system, which causes patient factors, such as airway resistance to have minimal impact on the air flow. HFNO systems are well suited for split airflow, substantially more so than invasive ventilators, CPAP, or BiPAP. Even so, the Airvo 2 is theoretically capable of supplying two patients with HFNO without impeding the maximum recommended levels of treatment according to major guidelines. Some hospitals, like Västmanland Hospital Västerås (where this project orginated), have subsequently modified these guidelines based on clinical experience to allow higher FiO2 as well as in some cases higher air flows. IDAS, as well as the Karolinska University Hospital both recommend limiting the HFNO air flow in COVID-19 patients to 30 litres / minute due to risk of aeorosolisation and the FiO2 to 50 % due to the risk of alveolar collapse. The Airvo is capable of outputting 2-60 litres / minute of airflow with 21-100% FiO2 and uses wholly proprietary connectors which are not readily available and cannot be used with standardised respiratory equipment. The main system in use outside of the ICU is the Fisher & Paykel Airvo 2, often called " Optiflow", which more precisely is the special nasal cannula used with the system. 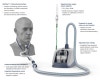
However, access to HFNO systems can be severely limited and scarcer than other equipment such as BiPAP machines. In the best case scenario, used in a timely and correct manner in the context of the COVID-19 pandemic, HFNO/HFNC can be used to avoid intubation and invasive ventilation. This is the case in Sweden (where this project was initiated), where the Infectious Diseases Association of Sweden ( IDAS, "Svenska Infektionsläkarföreningen" in Swedish) has recommended not using CPAP or NIV as well as limited upper maximums for HFNO (See below). High-Flow Nasal Oxygen (HFNO) / High Flow Nasal Cannula (HFNC) is a staple of treatment in COVID-19, especially as many countries, regions, hospitals, and health care providers are now recommending against regularly using CPAP and Non-Invasive Ventilation (NIV)/BiPAP in these patients. In the authors' limited experience the COVID-19 patients are often titrated to very similar treatments HFNO being a completely open system / circuit makes patient factors non significant for air flow dynamicsĭ. Using this only for cohort care with patients with the same disease makes cross contamination less significantĬ. Unidirectional high flow makes cross contamination unlikelyī. Treating two patients in parallell with HFNO using the Airvo 2 system is feasible due toĪ. The Airvo 2 system being capable of outputting 60 litres/minute (well above recommended maximum air flow) 
Treatment guidelines that stipulate a maximum flow should be kept as low as possible to avoid / minimise aerosol dispersion, often capped at 30 lpm.ī. 
A multicentre RCT comparing high-flow humidified oxygen and standard supplemental oxygen would be of benefit, as would including weaning strategies for high-flow humidified oxygen.Treating two patients in parallell with High-Flow Nasal Oxygen (HFNO) using the Airvo 2 system is possible due toĪ. The use of this medical device is becoming widespread without demonstration of additional efficacy. Newly-developed medical devices can now deliver high-flow humidified oxygen that is thought to provide more comfortable and effective delivery of gases while retaining airway humidity. Why this is important:- Providing oxygen (typically by nasal cannula) is standard care for bronchiolitis. High-flow humidified oxygen and oxygen:- What is the clinical and cost effectiveness of high-flow humidified oxygen versus standard supplemental oxygen? Any explanatory notes 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
